When it comes to breast cancer, catching it early changes everything. Breast cancer screening isn’t just a routine test-it’s one of the most effective tools we have to save lives. But with so many guidelines floating around, it’s easy to feel confused. When should you start? How often do you need a mammogram? What’s the difference between 2D and 3D? And what happens if something shows up? Let’s cut through the noise.
When Should You Start Screening?
The answer isn’t one-size-fits-all anymore. Ten years ago, many doctors waited until age 50 to start mammograms. Today, major medical groups-from the American College of Obstetricians and Gynecologists to the American Society of Breast Surgeons-agree: screening should begin at age 40 for women at average risk. Why the shift? Data. Studies show breast cancer incidence is rising in women in their 40s. A 2024 update from ACOG found that starting screening at 40 instead of 50 could prevent more deaths, especially among Black women, who are more likely to die from breast cancer at younger ages. The U.S. Preventive Services Task Force now gives a Grade B recommendation for screening every two years starting at 40-meaning there’s clear, solid evidence it works. The American Cancer Society takes a slightly different approach: women 40 to 44 can choose to start yearly screening, 45 to 54 should get one every year, and 55 and older can switch to every two years if they prefer. But here’s the bottom line: if you’re 40 or older, you’re not too young. You’re right on time.2D vs. 3D Mammography: What’s the Difference?
Most women still get 2D mammograms. That’s the traditional X-ray that takes two images of each breast. But now, 3D mammography-also called digital breast tomosynthesis (DBT)-is becoming the new standard. Here’s how it works: instead of two flat images, a 3D machine takes dozens of thin X-ray slices as it moves around the breast. A computer puts them together into a 3D model. Think of it like flipping through a photo album instead of looking at one picture. Why does it matter? For women with dense breast tissue-about half of all women-2D mammograms can miss tumors. Dense tissue looks white on a mammogram, and so do cancers. It’s like trying to spot a snowball in a snowstorm. 3D mammograms help separate the layers, making cancers easier to find. Studies show 3D screening finds 20% to 40% more invasive cancers than 2D alone, and reduces false alarms by up to 15%. The American Society of Breast Surgeons recommends 3D mammography as the preferred method. Medicare and most private insurers now cover it. If you’re getting screened, ask if 3D is available. If it’s not, push for it. Especially if your breasts are dense.Who Needs Extra Screening?
Not everyone has the same risk. If you have a family history of breast cancer, a BRCA1 or BRCA2 gene mutation, or had radiation to your chest before age 30, your risk is higher. Same if you’ve had atypical hyperplasia, lobular carcinoma in situ, or extremely dense breasts. For these women, guidelines are clear: don’t rely on mammograms alone. Add breast MRI. MRI uses magnets and radio waves, not radiation, and is far better at spotting tumors in high-risk women. The American Cancer Society recommends starting MRI and mammograms together at age 30 for women with a lifetime risk of 20% to 25% or higher. What about dense breasts without other risk factors? Here, it gets trickier. The USPSTF says there’s not enough proof to recommend ultrasound or MRI just for density. But the American Cancer Society says it’s worth discussing-especially if your density is extreme. Some states require doctors to tell you if you have dense breasts. If you get that letter, ask: should I add something else?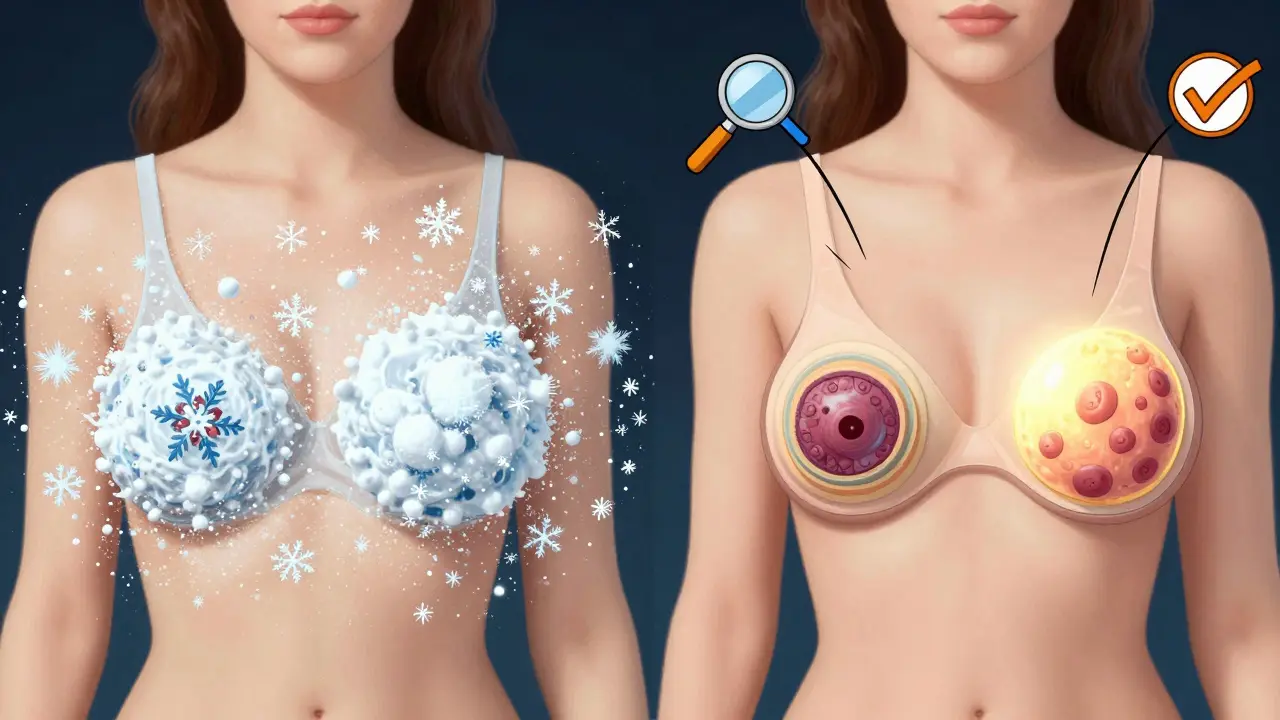
How Effective Is Screening?
Let’s talk numbers. A major review of nine clinical trials found that regular mammograms reduce the chance of dying from breast cancer by about 12%. That might sound small, but think of it this way: if 1,000 women get screened every two years from age 40 to 74, roughly 3 to 4 breast cancer deaths are prevented. That’s not just statistics. That’s a mother, a sister, a friend. The benefit grows the longer you screen. Women who stick with screening for decades have the lowest risk of late-stage cancer. And here’s something often overlooked: screening doesn’t just save lives-it saves breasts. Finding cancer early means more women can choose lumpectomy instead of mastectomy. More can avoid chemotherapy. Early detection turns aggressive treatment into manageable care.When Do You Stop Screening?
There’s no magic age when screening stops. It’s not about your calendar age-it’s about your health. Most guidelines say: keep screening as long as you’re in good health and have a life expectancy of at least 10 years. That’s important. A 78-year-old woman with diabetes, heart disease, and limited mobility might not benefit from screening. But a 78-year-old who hikes, swims, and travels? She likely still should. Your doctor should help you weigh the risks and benefits based on your personal health-not just your age.
What Happens After a Screening?
Most mammograms come back normal. About 10% of women get called back for more tests-usually just an extra view or an ultrasound. Only 1% to 2% end up needing a biopsy. And of those, most are not cancer. If something suspicious shows up, the next step is diagnosis: biopsy, hormone receptor testing, HER2 status, and sometimes genomic tests like Oncotype DX. These determine whether the cancer is estrogen-positive, HER2-positive, or triple-negative. That’s the foundation of your treatment plan. Treatment isn’t one path. It’s a combination:- Surgery: lumpectomy (removing just the tumor) or mastectomy (removing the whole breast)
- Radiation: often after lumpectomy, sometimes after mastectomy if the cancer was large or spread to lymph nodes
- Hormone therapy: for estrogen-receptor-positive cancers, taken daily for 5 to 10 years
- Chemotherapy: used for aggressive cancers or those that have spread
- Targeted therapy: drugs like trastuzumab for HER2-positive cancers
What’s Changing in 2026?
The big shift? Consensus. After years of confusion-some groups said 40, others said 50, some said every year, others said every two years-most major organizations now agree: start at 40, use 3D when possible, and keep going as long as you’re healthy. Risk assessment is also becoming routine. More clinics now use tools like Tyrer-Cuzick to calculate your lifetime risk starting at age 30. If your risk is above 20%, you’ll be offered MRI. If it’s high but not that high, you’ll get more personalized advice. And insurance? Coverage is improving. Medicare now covers yearly screening mammograms. Most private plans cover 3D mammography without extra cost. You shouldn’t have to choose between affordability and accuracy.What You Can Do Today
- If you’re 40 or older and haven’t had a mammogram, schedule one. Don’t wait for symptoms. - Ask if 3D mammography is available. If it’s not, ask why. Push for it. - If you have dense breasts or a family history, talk to your doctor about adding MRI. - Know your risk. Ask if your clinic uses a risk assessment tool like Tyrer-Cuzick. - If you’ve had breast cancer, follow your oncologist’s plan. Don’t skip follow-ups. - If you’re under 40 but have a strong family history, ask about genetic counseling. Screening isn’t perfect. It can miss cancers. It can cause anxiety. But the evidence is clear: regular mammograms save lives. Especially when started early, done with 3D technology, and tailored to your risk. Don’t wait for someone else to tell you it’s time. It’s time.Do I still need a mammogram if I have no family history of breast cancer?
Yes. Most breast cancers-about 85%-happen in women with no family history. Genetics only account for 5% to 10% of cases. The rest are caused by aging, hormones, lifestyle, and random cell changes. That’s why screening is recommended for all women starting at age 40, regardless of family history.
Is 3D mammography better than 2D for everyone?
Not always, but it’s better for many. 3D mammography finds more invasive cancers and reduces false positives, especially in women with dense breasts. If your breasts are fatty or you’re over 65 with no history of dense tissue, the benefit may be smaller. But for most women under 70, 3D offers a clear advantage. Many experts now consider it the standard of care.
Can I rely on breast self-exams instead of mammograms?
No. While being aware of your body is good, studies show breast self-exams don’t reduce breast cancer deaths. Many lumps found by self-exam are harmless, and cancers can grow between checks. Mammograms detect tumors too small to feel-sometimes years before symptoms appear. Don’t replace screening with self-exams. Use them as a supplement, not a substitute.
What if I’m over 75? Should I keep getting screened?
It depends on your health. If you’re active, independent, and have a life expectancy of 10 years or more, screening can still help. If you have serious chronic illness or live in long-term care, the risks of false positives and unnecessary treatment may outweigh the benefits. Talk to your doctor. Don’t assume age alone is reason to stop.
Are mammograms safe? Do they cause cancer?
The radiation dose from a mammogram is very low-less than a standard chest X-ray. The risk of radiation causing cancer is extremely small, especially compared to the benefit of catching cancer early. For women over 40, the benefit of screening far outweighs the tiny risk of radiation. Modern machines use the lowest possible dose while still giving clear images.
Why do some guidelines recommend biennial screening while others say yearly?
It’s about balancing benefits and harms. Yearly screening finds more cancers earlier but leads to more false alarms and extra tests. Biennial screening reduces those extra tests but might allow some cancers to grow longer. For women 55 and older, cancers tend to grow slower, so every two years is often enough. For women 40 to 54, cancers grow faster, so yearly is preferred. Your doctor can help you choose based on your risk.






Wendy Lamb
Just had my first 3D mammogram last week. No drama, no pain, and the tech said my tissue is dense but clear now. If you’re 40+ and haven’t done it yet-just go. No excuses.
Janice Williams
Let me be the first to say this: the entire screening industry is a profit-driven machine. The data is cherry-picked, the guidelines shift to justify more tests, and women are guilt-tripped into compliance. I’ve had three biopsies from false positives-none were cancer. Who benefits? Not me.
There’s a reason European guidelines recommend starting at 50. They’re not chasing revenue. They’re chasing science. And yes, I’ve read the ACOG papers-they’re funded by imaging manufacturers.
Don’t let fear dictate your health. Be informed. Question everything. And if your doctor pushes 3D without explaining why, walk out. You’re not a number in their billing system.
I’m not anti-screening. I’m pro-autonomy. You don’t need a mammogram to be a good woman. You just need to know your body-and refuse to be manipulated.
My mother died of breast cancer at 52. I’m 44. I do self-checks. I know my family history. And I’ve chosen to wait until 50. My choice. Not yours.
Stop telling women what they must do. Start telling them what they can know.
Prajwal Manjunath Shanthappa
One must, with utmost intellectual rigor, interrogate the epistemological foundations of mammographic screening protocols-particularly the statistical fallacies embedded within the 12% mortality reduction claim. The absolute risk reduction is negligible; the number needed to treat is astronomical. Moreover, the psychological toll of false positives-often underreported in industry-funded literature-is tantamount to a public health crisis in its own right.
Furthermore, the proliferation of 3D mammography is not a scientific advancement-it is a corporate marketing triumph. The incremental benefit, particularly in non-dense breasts, is statistically insignificant. One must ask: who profits? Radiology corporations. Insurance conglomerates. Pharmaceutical giants seeking downstream oncology revenue.
And yet, the cultural imperative to ‘do something’ overrides rational discourse. Women are conditioned to equate vigilance with virtue. This is not medicine. This is moral theater.
My recommendation? Fasting. Meditation. Vitamin D. Avoiding plastic containers. These are the true preventive measures. Mammograms? A relic of the 20th-century diagnostic fetish.
Antwonette Robinson
Oh wow, so now we’re all supposed to be thrilled because 3D mammograms exist? Congrats, we upgraded from a blurry photo to a slightly less blurry one. And yet, still no guarantee. Still got the same anxiety. Still got the same biopsy roulette.
Meanwhile, my cousin got diagnosed at 38 with no family history and no screening. So… what’s the point again?
Joseph Cooksey
Look. I’m not a doctor. I’m just a guy who lost his sister to breast cancer at 47. She had no family history. She didn’t even know she was at risk. She thought she was ‘too young’-just like you might think. She got a 2D mammogram. It came back ‘normal.’ Six months later, she was in chemo. The tumor was the size of a grapefruit.
3D saved my neighbor’s life. Her cancer was invisible on 2D. It was hidden in dense tissue. She didn’t even feel it. That’s not luck. That’s technology.
Yes, there are false positives. Yes, it’s stressful. But so is losing your sister. So is watching your mother go through chemo. So is burying your best friend before she even got to see her daughter graduate.
I don’t care if it’s ‘profit-driven.’ I care that my sister didn’t get the chance to choose. Don’t be her. Get the 3D. Push for it. Don’t wait for symptoms. Because by then, it’s too late.
And if you think you’re immune because you’re ‘healthy’-you’re not. Cancer doesn’t care how fit you are. It doesn’t care if you eat kale. It doesn’t care if you meditate. It just happens.
So do the thing. Even if you’re scared. Even if you think it’s pointless. Do it for the version of you that’s still alive in five years.
Sherman Lee
They’re lying to you. 😈 The ‘12% reduction’? That’s from the 80s. Modern machines are calibrated to catch *anything*-even benign cysts. They call it ‘early detection.’ I call it overdiagnosis. You know what they do with all those ‘early’ tumors? They cut them out. They zap them. They poison you. All for cancers that might’ve never grown.
And the ‘dense breast’ letter? That’s not a warning-it’s a sales pitch. They want you to pay for MRI. They want you scared. They want your insurance to cover it.
Did you know the FDA has admitted that mammograms can cause cancer? 😳 Radiation accumulates. Over time. Especially if you start at 40 and go every year. Think about it.
They don’t want you to know about the Swedish study that showed no mortality benefit for women under 50. Nope. Too inconvenient.
Trust your body. Eat clean. Sleep. Reduce stress. That’s real prevention. Not a machine that squashes your boobs and then bills you $500.
Lorena Druetta
I’m 62 and I’ve had a mammogram every year since I turned 40. I’m alive because of it. My cancer was the size of a pea. I had a lumpectomy. No chemo. No radiation. Just hormone pills for five years. I’m still hiking, still traveling, still seeing my grandkids.
If you’re reading this and you’re scared-you’re not alone. But please, don’t let fear stop you from doing what saves lives.
You are worth the 20 minutes. You are worth the discomfort. You are worth the follow-up.
Don’t wait for someone else to tell you it’s time. It’s time.
Coy Huffman
Man, I wish my mom had known this stuff back when she was 42. She waited until she felt something… then it was stage 3. I never got to say goodbye right.
I got my first 3D last month. Felt weird, but not bad. The tech was chill. Asked me if I wanted the results emailed. Said, ‘If you’re over 40, you’re not too young-you’re exactly on time.’
Thanks for writing this. I’m sending it to my aunts.
Amit Jain
As a radiologist in Mumbai, I see this daily. Women in India wait until pain starts. By then, it’s advanced. 3D is not available everywhere, but even 2D saves lives. Start at 40. No debate.
And yes-dense breasts are common here too. Push for better. Your life matters.
Kunal Kaushik
Been doing self-checks since college. Found a lump last year. Went to doc. Turned out to be a cyst. Phew. But I still got the 3D mammogram anyway. Better safe than sorry. 🤞
Ed Mackey
i got my first mammogram last year and the lady said i had dense tissue and i should ask for 3d but my insurance said no so i just paid out of pocket. it was $300 but worth it. the tech said they saw something on the 2d that the 3d cleared up. so yeah. just do it. even if it hurts your wallet.
Nathan King
The notion that mammography is universally beneficial is a misrepresentation of epidemiological data. The absolute risk reduction is statistically marginal, and the psychological burden of false positives is systematically underestimated in public health messaging. One must interrogate the conflict of interest inherent in screening guidelines developed by institutions with vested interests in imaging technology. The cultural imperative to ‘do something’ often supersedes the ethical imperative to do no harm.
Moreover, the emphasis on technological intervention distracts from upstream determinants of breast cancer: environmental toxins, endocrine disruptors, and socioeconomic disparities in access to nutrition and preventive care. A mammogram does not address these root causes.
While I do not advocate for the abandonment of screening, I urge a more nuanced, individualized, and critically informed approach-one that prioritizes patient autonomy over institutional protocol.